
If you live with a stoma, there is one worry that quietly sits in the back of most ostomates’ minds: the risk of a parastomal hernia. Research suggests that somewhere between 30% and 50% of people with a stoma will develop one within a few years of surgery, and that number climbs the longer you have your stoma. It is, by some measures, the most common long-term complication of ostomy surgery.
The good news is that parastomal hernias are not inevitable, and many of the habits that reduce your risk are well within your control. This guide walks through what a parastomal hernia actually is, why they happen, who is most at risk, and the practical day-to-day steps you can take to lower your chances of developing one. Everything here is written for real life, not a medical textbook.
Key Takeaways
- A parastomal hernia happens when part of the intestine or abdominal tissue pushes through the weakened muscle around your stoma.
- Up to half of ostomates develop one, but risk can be meaningfully reduced with support, smart movement, and weight management.
- Wearing an abdominal support belt, especially during lifting, coughing, or exertion, is one of the simplest and most recommended prevention strategies.
- Avoid heavy lifting for at least 6 to 8 weeks after surgery, then rebuild core strength gradually with guidance.
- Call your ostomy nurse or surgeon if you notice a new bulge, changes in pouching fit, or pain around the stoma.
What Is a Parastomal Hernia?
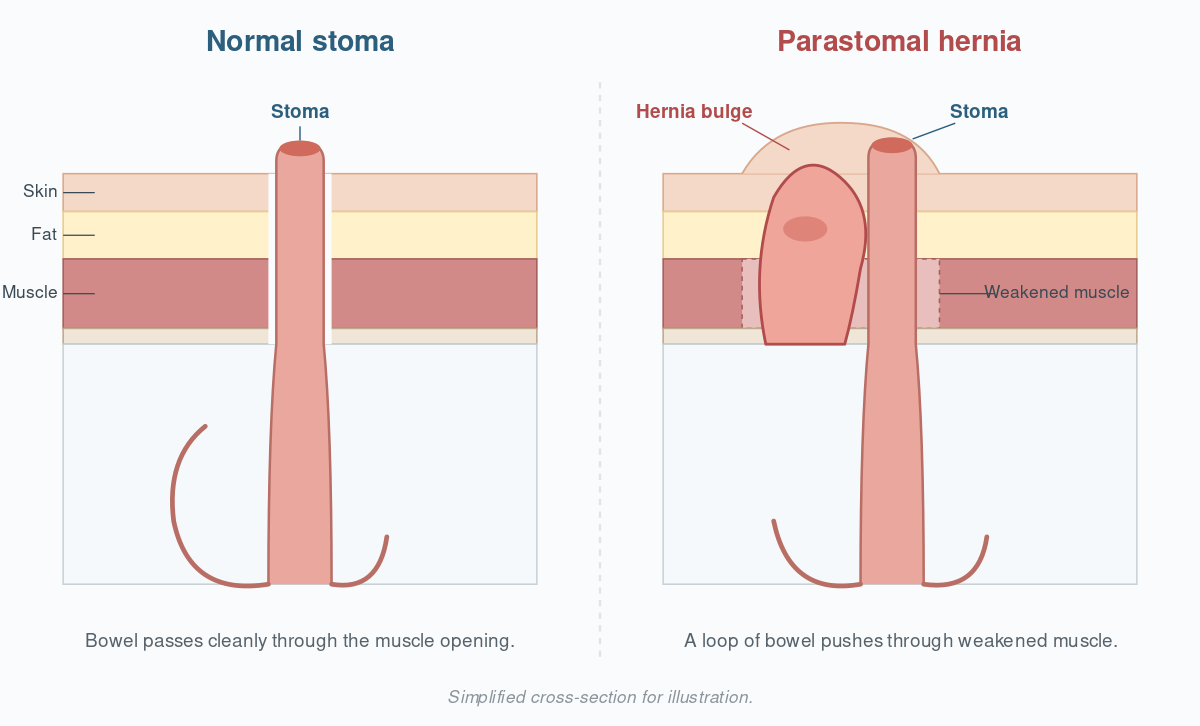
A parastomal hernia is a specific type of incisional hernia. During stoma surgery, the surgeon creates an opening in the abdominal wall so the bowel can be brought to the skin’s surface. That opening never fully closes, because the stoma passes through it. Over time, the muscle around that opening can weaken, and a loop of bowel or fatty tissue can start to push through alongside the stoma.
On the outside, you usually notice a parastomal hernia as a soft bulge or swelling around the stoma. It may be more obvious when you stand, cough, or strain, and it may flatten when you lie down. Some hernias cause no symptoms at all and are only spotted during a checkup. Others make pouching harder, cause discomfort, or in rare cases lead to a serious complication where the bowel gets trapped. That is why early awareness matters.
Find My Stoma Stifler Setup
Why Do Parastomal Hernias Happen?
Anyone who has had ostomy surgery has a slightly weakened spot in the abdominal wall by design. A parastomal hernia develops when the pressure inside the abdomen, combined with time and tissue weakness, overcomes the structural integrity of that spot. Several factors raise the odds:
- Natural muscle weakening with age. Tissue loses elasticity over time, which is one reason hernia risk rises the longer you have your stoma.
- Extra abdominal pressure. Anything that repeatedly pushes outward from inside the abdomen adds stress to the stoma site. Heavy lifting, chronic coughing, constipation-related straining, and pregnancy are common culprits.
- Excess weight, especially around the midsection. More abdominal fat means more constant outward pressure on the stoma site.
- Surgical factors. The size of the original stoma opening, how it was placed, and whether mesh was used all influence baseline risk. This is something your surgeon considered at the time.
- Underlying conditions. Diabetes, smoking, and long-term steroid use can slow tissue healing and weaken the abdominal wall.
The takeaway is that hernia risk is a combination of things you cannot change (like age or the original surgery) and things you absolutely can (like daily habits, weight, and support).
Who Is Most at Risk?
You are at higher risk of developing a parastomal hernia if you fit any of these:
- Had ostomy surgery more than 2 years ago
- Carry extra weight, particularly around the abdomen
- Have a job or hobby that involves frequent lifting or heavy physical exertion
- Have a chronic cough (from smoking, asthma, or another cause)
- Have a history of other hernias or weakened connective tissue
- Deal with frequent constipation and straining
If that list describes you, it does not mean a hernia is certain. It means the prevention strategies below matter more for you than for someone without those factors.
How to Prevent a Parastomal Hernia: What Actually Works
The research and clinical guidance around parastomal hernia prevention keeps returning to the same handful of strategies. None of them are dramatic. All of them add up.
1. Wear an Abdominal Support Belt
This is consistently the most-recommended prevention strategy from ostomy nurses, and for good reason. A proper stoma support belt gently compresses the abdomen, which does two things. First, it supports the weakened muscle around your stoma so less pressure lands directly on that spot. Second, it creates a physical reminder of your core during activity, so you are less likely to strain in ways that put your stoma at risk.
Support belts are particularly important during:
- Lifting, even lifting that feels light (groceries, a laundry basket, a small child)
- Exercise and sports
- Gardening, housework, and any bent-over activity
- Coughing or sneezing fits
- Anything that makes you brace your abdomen
A belt is not a brace you only wear when injured. For many ostomates, it becomes part of the daily routine, similar to wearing sunscreen or taking a daily vitamin. Start early, before a hernia shows up, not after.
Stoma Stifler™ Kit

Our complete abdominal support kit includes the molded Stoma Stifler cup, anchor plate, long and short Snug Bands with adjustable clips, and hook-and-loop roll. Designed to protect your stoma and support the surrounding muscle during daily activity, exercise, and lifting.
Shop The Kit2. Protect Your Core After Surgery
The first 6 to 8 weeks after ostomy surgery are the highest-risk window. Your body is laying down the scar tissue that determines the long-term strength of the stoma site. During this period, most surgeons will tell you to avoid lifting anything heavier than about 10 pounds, which is lighter than a gallon of milk. It is tempting to push through once you feel better, but tissue healing is slower than pain relief. Stick to the rules your surgical team gave you, even when you feel up to more.
After your surgeon clears you, continue to be thoughtful about how you lift. Keep the weight close to your body. Use your legs, not your back. Exhale on effort. And when in doubt, wear your belt.
3. Build Core Strength the Right Way
This one surprises people. The old advice was often “do not work your core at all after a stoma.” Current thinking is more nuanced. A weak, deconditioned core actually raises hernia risk over time because the muscles surrounding the stoma site have less support. The goal is to rebuild core strength gradually, with the right kinds of exercises, and to avoid moves that spike abdominal pressure.
Generally safer choices include gentle walking, swimming once your surgical site has fully healed, stationary biking, and specific pelvic floor and deep abdominal exercises taught by a physical therapist who understands ostomies. What to avoid, at least without professional guidance, includes heavy crunches, loaded sit-ups, heavy deadlifts, and anything that causes you to bulge or bear down.
If you can see an ostomy-aware physical therapist or rehab specialist once, it is some of the best money you can spend. They will give you an individualized plan that is safer than anything a generic video can offer.
4. Manage Your Weight, Especially Around the Midsection
Extra abdominal weight is one of the strongest predictors of parastomal hernia development. Every extra pound in that region adds constant outward pressure on the stoma site. Weight management is rarely simple, and for ostomates it is complicated further by dietary restrictions, medication, and energy levels. Small, sustainable changes beat aggressive plans.
Even a modest reduction in abdominal weight can lower hernia risk. Focus on gentle daily movement, adequate protein, and the foods your stoma tolerates well. If weight has been difficult to manage since surgery, a registered dietitian familiar with ostomy nutrition can be a real help.
5. Learn Proper Body Mechanics for Everyday Life
A surprising amount of hernia risk comes not from the gym but from ordinary moments: getting up from a low couch, picking up a pet, loading a dishwasher, putting a suitcase in an overhead bin. The body mechanics that protect your stoma are the same ones that protect your back:
- Bend at the knees, not the waist
- Keep objects close to your body when you lift
- Exhale as you exert effort (never hold your breath)
- Ask for help with anything unusually heavy or awkward
- Get up from sitting by sliding to the edge of the seat and pressing through your legs, not by doing a sit-up motion

These habits take a few weeks to become automatic. Once they do, they protect you for life.

Stoma Stifler™ — The Sound Suppressor + Stoma Guard Most Ostomates Wish They’d Found Sooner
6. Address Chronic Cough and Constipation
Both create repeated spikes of abdominal pressure. A chronic cough, whether from smoking, allergies, or a medication side effect, deserves a proper workup. Constipation is manageable with hydration, fiber from foods your stoma tolerates, and, when necessary, advice from your ostomy team about stool softeners. Neither of these should just be accepted as background noise when you have a stoma. They directly raise hernia risk.
When to Call Your Ostomy Nurse or Doctor
See your team if you notice any of the following around your stoma:
- A new bulge, swelling, or asymmetry, even if it is not painful
- Changes in how your pouching system fits, unexplained leaks, or skin irritation
- Pain, pressure, or discomfort around the stoma
- Nausea, vomiting, or no output from the stoma (call urgently, this can indicate a trapped bowel loop)
Most parastomal hernias are managed with support belts and lifestyle adjustments rather than surgery. Catching one early gives you the widest set of options.
The Bottom Line
Parastomal hernias are common, but they are not a guarantee. The daily habits that reduce risk, including wearing a proper support belt, lifting smart, rebuilding core strength with care, and managing abdominal pressure, compound over months and years. None of them require a dramatic lifestyle overhaul. They just require consistency.
If you are newly stoma’d, starting these habits now is easier than adding them later. If you have had your ostomy for years and want to reduce your risk going forward, it is never too late. Protect the site, support the muscle, and stay in conversation with your ostomy team. Your future self will thank you.
For more on everyday stoma life, you may also like our posts on what causes a prolapsed stoma and how to address it, adjusting to life after ostomy surgery, and practical tips for managing stoma noise.
This article is general education, not medical advice. If you are worried about a hernia or have had ostomy surgery recently, please talk with your ostomy nurse or surgeon about what makes sense for your situation.
Helpful products on Amazon
These are the products stoma nurses and the ostomy community consistently mention for hernia prevention and management. The links go to tagged Amazon searches so you can compare options.
Affiliate disclosure: This article contains Amazon affiliate links. As an Amazon Associate we earn from qualifying purchases — at no extra cost to you. Recommendations are based on what stoma nurses and the ostomy community consistently mention; the links go to tagged Amazon searches so you can compare options rather than being pushed toward a single product. Read our full disclosure here.
Frequently Asked Questions
Is what I'm experiencing normal after ostomy surgery?
Most concerns ostomates have – bag noise, gas, occasional leaks, skin irritation, body-image adjustment – are normal in the first 6-12 months. The frequency and intensity drop significantly as your body adapts and your routine settles. Reach out to your ostomy nurse if anything feels worsening rather than improving.
When should I call my ostomy nurse or doctor?
Call promptly for: peristomal skin that's painful, bleeding, or breaking down; stoma color changes (dusky, purple, pale); no output for 4-6 hours with cramping (possible blockage); high output that won't slow despite reducing fiber and adding electrolytes; or a hernia bulge that becomes painful or won't reduce. Most other concerns can wait for your next scheduled appointment.
Does the Stoma Stifler help with this?
The Stoma Stifler is designed to quietly absorb gas and reduce bag noise without restricting output. It works with your existing pouching system and doesn't interfere with skin care or wafer adhesion. Pairing it with the basics – good skin routine, hydration, and any complementary supplies above – covers most daily-comfort challenges.
Helpful complementary supplies
A few items most ostomates keep on hand. These pair with your Stoma Stifler for an easier daily routine.







